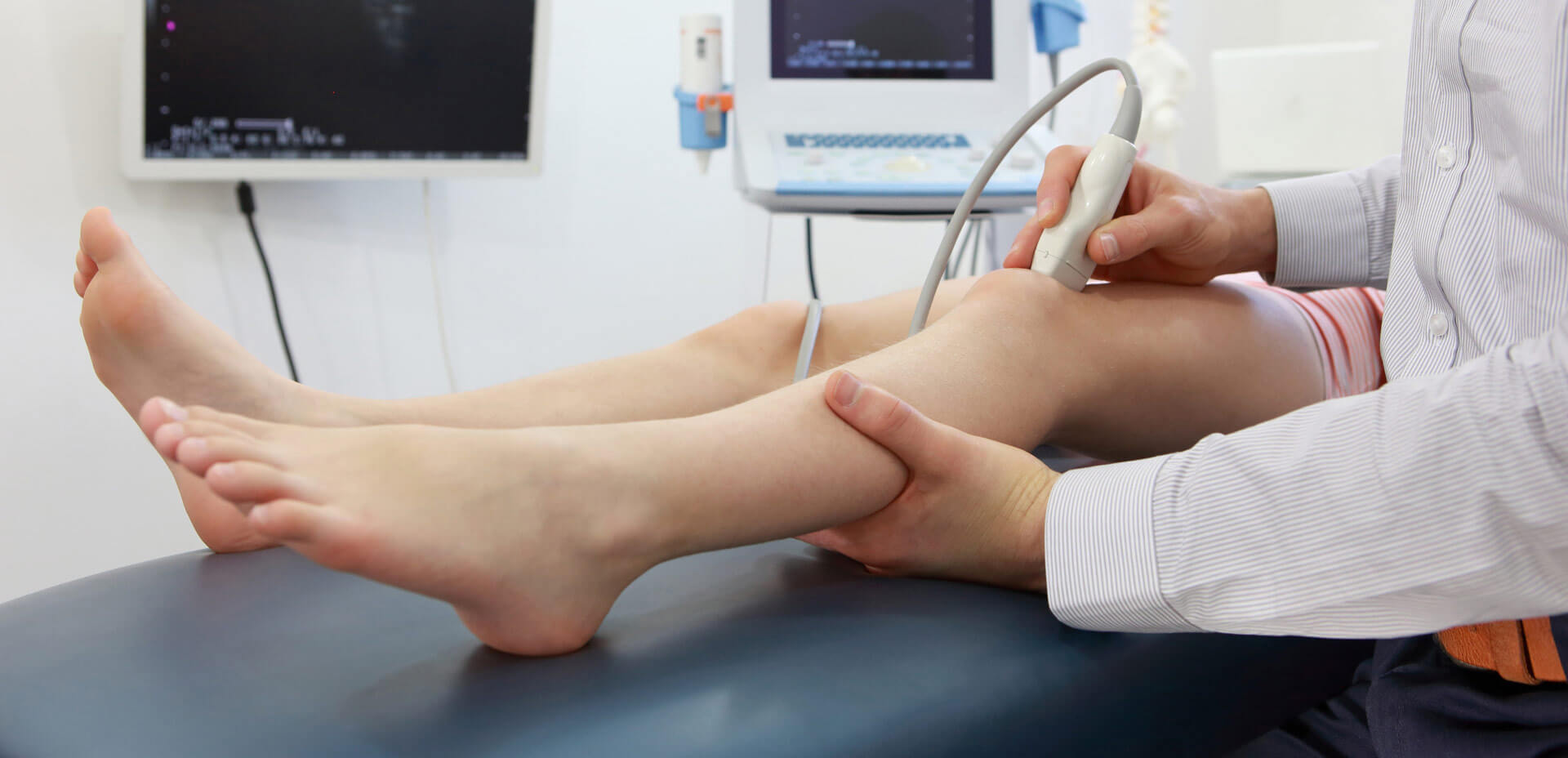
MAKO Robotic Arm Assisted Knee Replacement
Mr Pavlou is the first surgeon on the South Coast to perform robotic arm assisted Total knee replacement, making use of a MAKO robotic arm.
Before the surgery, you will have a CT scan which generates a 3D model of the area to be operated on. This model is used to create a personalised surgical plan based on your anatomy and will indicate the optimal size and placement of your implants, which is vital for correct biomechanical reconstruction.
During the operation the robotic system guides the surgeon based on the personalised pre-operative plan and prevents them from moving outside of pre-defined boundaries; however, the surgeon can alter the plan intraoperatively as necessary based on real-time information. The guidance provided by the system means that the surgeon is able to remove the diseased bone while preserving the surrounding healthy bone and tissue.
The robotic system allows for much more accurate placement of your implants compared to traditional methods, meaning that you will have a more natural feeling knee post knee replacement.
The benefits of using the robot include a smaller incision, less pain and faster recovery times; restoring your confidence in your mobility and helping you to return to your active lifestyle within weeks. Additionally, the lifetime of implants is dictated by the accuracy of placement, with more accurately positioned implants lasting longer. Therefore, replacement surgeries performed using the robot are likely to last longer and so result in greater patient satisfaction.

Knee Realignment Surgery
Knee realignment surgery can be used as an alternative to joint replacement to treat selected cases of osteoarthritis of the knee.
In the most common form of knee arthritis only one side of the knee joint cartilage becomes damaged. This is usually because more than half of the forces going trough the knee joint travel through the inner aspect of the knee, leading to increased wear.
By realigning the long axis of the lower limb the forces going through the knee can be directed from the worn side of the knee to the unworn side, relieving pain without the need for major reconstructive surgery.
The surgery usually provides lasting relief for approximately 10 years, after which a joint replacement in usually required.
Knee realignment surgery is usually reserved for more active patients and is not suitable for all types of knee arthritis. Mr Pavlou would be happy to discuss whether this is a suitable option for the treatment of your knee arthritis.
Mr Pavlou would be happy to discuss whether this is a suitable option for the treatment of your knee arthritis.


Revision Knee Replacement
Revision Knee Replacement means that part or all of your previous knee replacement needs to be replaced (revised).
This operation varies from very minor adjustments to massive operations replacing significant amounts of bone. The typical knee replacement replaces the ends of the femur (thigh bone) and tibia (shin bone) with plastic inserted between them and usually the patella (knee cap).
Do I need my knee replacement revised?
If you have had a knee replacement in the past and you have developed pain, instability or deformity you may need your knee replacement revised. Mr Pavlou will be able to offer you expert advise on the management of a painful knee replacement.
Why does a knee replacement need to be revised?
Pain is the primary reason for revision. Usually the cause is clear but not always. Knees without an obvious cause for pain in general do not do as well after surgery.
Plastic (polyethylene) wear – This is one of the easier revisions where only the plastic insert is changed.
Instability – This means the knee is not stable and may be giving way or not feel safe when you walk.
Loosening of either the femoral, tibial or patella component – This usually presents as pain but may be asymptomatic. It is for this reason why you must have your joint followed up for life as there can be changes on X-ray that indicate that the knee should be revised despite having no symptoms.
Infection- usually presents as pain but may present as swelling or an acute fever.
Osteolysis (bone loss). This can occur due to particles being released into the knee joint that result in bone being destroyed.
Stiffness- This is difficult to improve with revision but can help in the right indications.
Risks and Complications
As with any major surgical procedure there are risks involved. The risks and complications are similar to your original knee replacement but occur slightly more frequently. Mr Pavlou will cover these in detail prior to any surgical procedure and provide you with clear written information of the risks and benefits of surgery.

Shockwave Therapy
What is shock wave therapy?
ESWT, also known as Shockwave Therapy, provides treatments to patients suffering from a range of chronic conditions such as Patellar Tendinopathy and trochanteric bursitis of the hip that are notoriously difficult to resolve.
How does it work?
The basic principles behind shockwave therapy are the high pressured acoustic shockwaves that travel through the skin to stimulate pain relief and tissue repair.
What does it involve?
Mr Pavlou will pass the shockwave applicator over the injured area. While the stimulation may produce some discomfort, patients often feel immediate reduction of pain in the first 24 hours after treatment.
How many treatments will I need?
The therapy usually involves 3 sessions of 10 to 15 minutes
Knee Arthroscopy
What is it?
Arthroscopy is commonly known as “key-hole” surgery. The arthroscope is a small fiber-optic telescope attached to a camera, which is inserted into a joint to evaluate and treat a number of conditions. The picture is visualized on a TV monitor. The benefits of arthroscopy involve small incisions (hence “key-hole”), faster healing, a more rapid recovery, and less scarring.
Most arthroscopic surgery is performed as day surgery and is usually done under general anesthesia. It is even possible to have the surgery whist you are awake watching Mr Pavlou perform your surgery.
Do I need arthroscopy?
The most common reason to have a knee arthroscopy is to treat a damaged meniscal (“shock-absorbing”) cartilage, which is still causing pain and mechanical symptoms despite other non-surgical treatments. Other common conditions amenable to arthroscopic treatment include damaged surface cartlilage, loose bodies in the knee, knee-cap problems and removal of painful abnormal folds (plicae) within the knee.
Before considering a knee arthroscopy Mr Pavlou will take a detailed history and perform a thorough physical examination. You are likely to need further tests such as an MRI scan, which in addition to Mr Pavlou’s expert clinical assessment will help guide your treatment.
What are the risks?
The risks and complications of arthroscopic knee surgery are extremely small. However, it is imperative that you are aware of the common risks. Mr Pavlou will go through these with you in detail and also provide you with a detailed information sheet.
Risks related to Arthroscopic Knee Surgery Include:
- Postoperative bleeding
- Deep Vein Thrombosis
- Infection
- Stiffness
- Numbness to part of the skin near the incisions
- Injury to vessels, nerves and a chronic pain syndrome
- Progression of the disease process
One must also bear in mind that occasionally there is more damage in the knee than was initially thought and that this may affect the recovery time. In addition if the cartilage in the knee is partly worn out then arthroscopic surgery has about a 65% chance of improving symptoms in the short to medium term but more definitive surgery may be required in the future. In general arthroscopic surgery does not improve knees that have well established Osteoarthritis.
How did my surgery go?
Before you are discharged home Mr Pavlou will explain his findings and what treatment was required. He will show you high-resolution pictures and you may even keep a copy of these should you so wish. Don’t worry if it’s a lot to take in all at once, he will go through it all again in you follow up appointment.
Post – Operative Exercises and Physical Therapy
Following your surgery you will be seen by a physiotherapist and given an instruction sheet showing exercises that are helpful in speeding up your recovery. Strengthening your thigh muscles (Quadriceps and Hamstrings) is most important. Swimming and cycling (stationary or road) are excellent ways to build these muscles up and improve movement.
FAQs
How long does the surgery take?
Usually 20-30 minutes.
How long am I in the Hospital?
Approximately 4 hours.
Do I need crutches?
Usually not required (unless you are having ACL Reconstruction or meniscal repair).
When can I get the knee wet?
After 24 hrs remove the bandage and apply a waterproof dressing.
When can I drive?
After 24 hrs if the knee is comfortable.
When can I return to work?
This depends a little on what job you do. Usually 2-4 weeks, when the knee feels reasonably comfortable.
When can I swim?
After removal of the paper stitches.
How long will my knee take to recover.
Depending on the findings and surgery, usually 4 to 6 weeks following the surgery.
When can I return to Sports?
Depending on the findings, 4-6 weeks after surgery.